Category Archives: Internal
End Stage Renal Disease Patients, Doctors and Trust
End Stage Renal Disease (ESRD) patients require different level of attention and different level of trust between doctor and patient. For several reasons. They can weaken quickly. Imagine they walk to dialysis room and soon after they get getting to dialysis they get sleepy and tired. They feel drained. They feel no energy is left. They walk in with smile and they leave with a tired face. Doc has to understand it. We should brief for them what happened during their dialysis while they were sleeping through it. It helps them to feel and become part of this treatment. If they look too tired after dialysis and they do not want to talk as much, that does not mean that they are moody patients. It may mean that they just got very drained.
They have pain in their body. All over the body. It is real. We need to believe that. Hyperparathyroidism, osteomalacia (while phosphorus is high), microfractures, adynamic bone disease, muscle spasms, muscle necrosis and atrophy, being irritable, constant puncturing of the veins and vascular accesses, chronic pain syndrome, neuropathy, side effects of medications, chronic nausea due to medications and the disease, depression, lack of sleep at the right time, restless leg syndrome, falls, and several other reasons induces either chronic pain or low threshold to pain in these patients. These are real. We need to understand it, believe it, and be with them when they need us to help them with their condition.
Blood flow and volume removal adjustments. It really matters. It matters on one side to get the best KT/V and fluid adjustment. And on the other side most of patients symptoms during dialysis is just because of different rates of blood flow and volume removal. A smart dialysis patient senses changes in the body and associates it with changes in blood flow and fluid removal rate. They learn that different filter may have different fluid removal and dialysis profile. We better respect their opinion. They always have a point. Slow down the speed of your round doc, and listen to your patient. You may know the formula but remember you are applying it to their body. Be patient and understand they have the right to know what is going on. Do not get mad easily and do not tell you are the doctor because you are the doctor for the patient and patient needs to know what the deal is.
Trust and confidence is specially very critical issue at the time we need to decide about initiation of dialysis. Try to earn it. Very critical time. Remember we are telling a patient that your life is going to completely change. Completely. You will have several hours a week that does not belong to you anymore. It belongs to dialysis. You will have no urine after a while. You will be dependent on this machine in order to survive. We know our hands and legs belong to ourselves. And we know we have some organs in the body. Now we are telling the patient you have another organ which is not in you. It is next to you. Which you do not control it, the medical group controls it. And in order to get a good result you need to follow the advice of medical group. Trust me, these are major life changes. Give the patient some time to get through this major challenge of signing in for a dependency. They only do it because there is no other option at that time. As medical professionals we need to know that we should put a patient in this dependency only if it is vital. On the other hand we should not delay till they get harmed.
Understand that major certain elements of a normal person’s life is seriously damaged in a patient with ESRD. Daily activities, jobs, sex, relationship, endurance, persistency, independency, and many things are all poorly functioning or totally disabled in these patients. These patient are still so strong that they can smile. Remember this when you see them being nice to you. They are trying to be hero. They are trying to be successful in dealing with these new challenges while their resources are getting very limited. They should look at you as resource. Again try to earn it. We have to have respect for these heroes.
Our new lives as doctors and medical professionals with limitations of bundling and so on. As much as possible choose the best for your patient. If you can share with them the options in a realistic way. It does not help the patient if we tell them the only thing that can help them is for example drug A and we cannot write it due to limitations of bundling. If drug A is that important do your homework first. Talk to the dialysis company or patient’s social worker and insurance. See if you can arrange it. There might be a way to get it available. Do not put all the burden on the patient. They are already looking at life through a very small hole in the door. Do not close up that hole.
Alireza Atef, MD, Dallas, Texas
24-hour Urine Test Instructions for Outpatients
Instructions on how to collect 24-hour urine tests in the outpatient settings (outside the hospitals). We suggest you choose a day that you are not very busy and it can be convenient for you to collect every drop of urine during that 24 hour. Start time can be any time but it will be more convenient for you to start from the time you wake up that day (lets call it Day First). Suppose you wake up at 6 in the morning and you have the urge to urinate. Void the way you normally do. That urine does not need to be collected. Flush down that urine as you normally do. Any urine after that should be collected for 24 hour.
Male patients can directly urinate in the jar provided by the clinic or laboratory. Female patients need to void in a urine specimen toilet collection hat and them empty it in the jar.
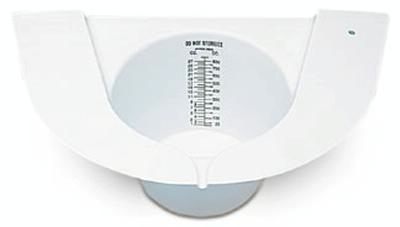
Urine specimen collection hat
If there is stool in the collection hat as well, you can still collect that urine but try not to mix the stool with urine and do not drop the stool in the jar.
During this 24-hour keep the jar either in refrigerator or in a cool box in contact with ice.
You should wake the next day (lets call it Day Two) the same time as you did on Day First (in this example at 6 am). You need to void at this time as you did in the rest of that 24-hour. It means this urine should be collected. Do not flush down this last urine.
This concludes the collection procedure.
Drop the jar at the clinic or laboratory the same day.
This technique will not be useful if you have no control over your urination (urinary incontinence) and you use diaper. In this case a urinary catheter should be inserted in the bladder for collection. Inform your physician about your urinary incontinence.
In patients who have gone through surgery on their bladder and have urostomy bag, 24 hour urine can be collected as above. At the start time, dump the urine in the bad and collect any urine after that for 24 hours as instructed.
Once a patient asked me...
Once a patient asked me, “how did you know I take Clonidine?” This is a real experience. I had a patient who had high blood pressure but his blood pressure (BP) was far from becoming stable and his BP reading was only in the acceptable range for few hours of a day but immediately after is was very high again. Whenever I see a chart like this, I ask the patient if he or she is taking clonidine. And it is very common to hear that patients state they are on clonidine. About an hour after taking clonidine (orally) blood pressure starts dropping. This effect will not last for more than few hours. In majority of cases blood pressure then increases to levels even more than what is was before taking clonidine.
Soon after its clinical use in 1964, it was noticed that stopping clonidine can cause rebound hypertension.
Fifty years later we still face a large number of patient who are on clonidine and suffer large swings in their BP.
This wide BP swings can be very detrimental and is not without harm.
(http://www.ncbi.nlm.nih.gov/pubmed/7011348 and http://www.ncbi.nlm.nih.gov/pubmed/4005090)
In my practice I try to take every patient off clonidine if possible.
Eating fish gives older adults an edge
Researchers found that older adults who had the highest omega-3 blood levels lived an average of 2.2 years longer than those with lower levels. “The findings suggest that the biggest bang for your buck is for going from no intake to modest intake, or about two servings of fatty fish per week,” said Dariush Mozaffarian, associate professor in the Department of Epidemiology at HSPH. Older adults who have high blood levels of omega-3 fatty acids — found almost exclusively in fatty seafood — may be able to lower their overall mortality risk by as much as 27 percent and their mortality risk from heart disease by about 35 percent, according to a new study from Harvard School of Public Health (HSPH) and the University of Washington. Researchers found that older adults who had the highest blood levels of the fatty acids lived, on average, 2.2 years longer than those with lower levels.
“Although eating fish has long been considered part of a healthy diet, few studies have assessed blood omega-3 levels and total deaths in older adults,” said lead author Dariush Mozaffarian, associate professor in the Department of Epidemiology at HSPH. “Our findings support the importance of adequate blood omega-3 levels for cardiovascular health, and suggest that later in life these benefits could actually extend the years of remaining life.”
The study — the first to look at how objectively measured blood biomarkers of fish consumption related to total mortality and specific causes of mortality in a general population — appeared online today in Annals of Internal Medicine.
Previous studies have found that fish, which is rich in protein and heart-healthy fatty acids, reduces the risk of dying from heart disease. But the effect on other causes of death or on total mortality had been unclear. With this study, the researchers sought to paint a clearer picture by examining biomarkers in the blood of adults not taking fish oil supplements, to provide the best assessments of the potential effects of dietary consumption of fish on multiple causes of death.
The researchers examined 16 years of data from about 2,700 Americans aged 65 or older who participated in the Cardiovascular Health Study (CHS), a long-term study supported by the National Heart, Lung, and Blood Institute. Participants came from four communities in North Carolina, California, Maryland, and Pennsylvania, and all were generally healthy at baseline. At baseline and regularly during follow-up, participants had blood drawn, underwent physical examinations and diagnostic testing, and were questioned about their health, medical history, and lifestyle.
The researchers analyzed the total proportion of blood omega-3 fatty acids, including three specific ones, in participants’ blood samples at baseline. After adjusting for demographic, cardiovascular, lifestyle, and dietary factors, they found that the three fatty acids — both individually and combined — were associated with a significantly lower risk of mortality. One type in particular, docosahexaenoic acid, or DHA, was most strongly related to lower risk of death from coronary heart disease (CHD) (40 percent lower risk), especially CHD death due to arrhythmia (an electrical disturbance of the heart rhythm) (45 percent lower risk). Of the other blood fatty acids measured, eicosapentaenoic acid (EPA) and docosapentaenoic acid (DPA), DPA was most strongly associated with a lower risk of stroke death, and EPA most strongly linked to a lower risk of nonfatal heart attack. None of these fatty acids were strongly related to other, non-cardiovascular causes of death.
Overall, the study participants with the highest levels of all three types of fatty acids had a 27 percent lower risk of total mortality due to all causes.
When the researchers looked at how dietary intake of omega-3 fatty acids related to blood levels, the steepest rise in blood levels occurred when intake increased from very low to about 400 mg per day; blood levels rose much more gradually thereafter. “The findings suggest that the biggest bang for your buck is for going from no intake to modest intake, or about two servings of fatty fish per week,” said Mozaffarian.
Support for the study came from the National Heart, Lung, and Blood Institute and the Office of Dietary Supplements of the National Institutes of Health.
